What Causes Adult Acne? Symptoms, Triggers, and Treatment Options
Adult acne is often assumed to be a continuation of teenage skin concerns, but in reality, many people experience breakouts for the first time in their twenties, thirties, or later. It is a common and clinically recognised condition, yet it remains widely misunderstood.
Compared to adolescent acne, adult acne tends to follow different patterns. It may respond differently to treatment, appear in different areas of the face, and often requires a more considered, medically informed approach. For many, it becomes not just a skin concern, but something that affects confidence and overall wellbeing.
In most cases, adult acne is not caused by a single factor. It usually develops as a result of several overlapping influences, including hormonal changes, skin physiology, and certain lifestyle or environmental triggers.
This article explains what adult acne is, how it typically presents, what causes it, and which treatment options are considered effective in a clinical setting, particularly within private clinics in London. It also outlines when it may be helpful to seek advice from a dermatology specialist.
How Is Adult Acne Different from Teenage Acne?
Adult acne refers to acne that continues beyond the age of 25 or develops for the first time in adulthood. Although the underlying processes are similar to those seen in adolescent acne, the way it presents is often different.
In adults, breakouts are more likely to appear on the lower part of the face, particularly the jawline, chin, and neck. These spots tend to be deeper, more inflamed, and slower to settle. Rather than occasional flare-ups, adult acne often follows a more persistent or recurring pattern.
Another important distinction is that adult acne is more closely linked to hormonal fluctuations and chronic triggers. It may also occur alongside other skin concerns, such as sensitivity, dryness, or changes in pigmentation, which can influence both how the skin behaves and how it responds to treatment.
Common Symptoms of Adult Acne
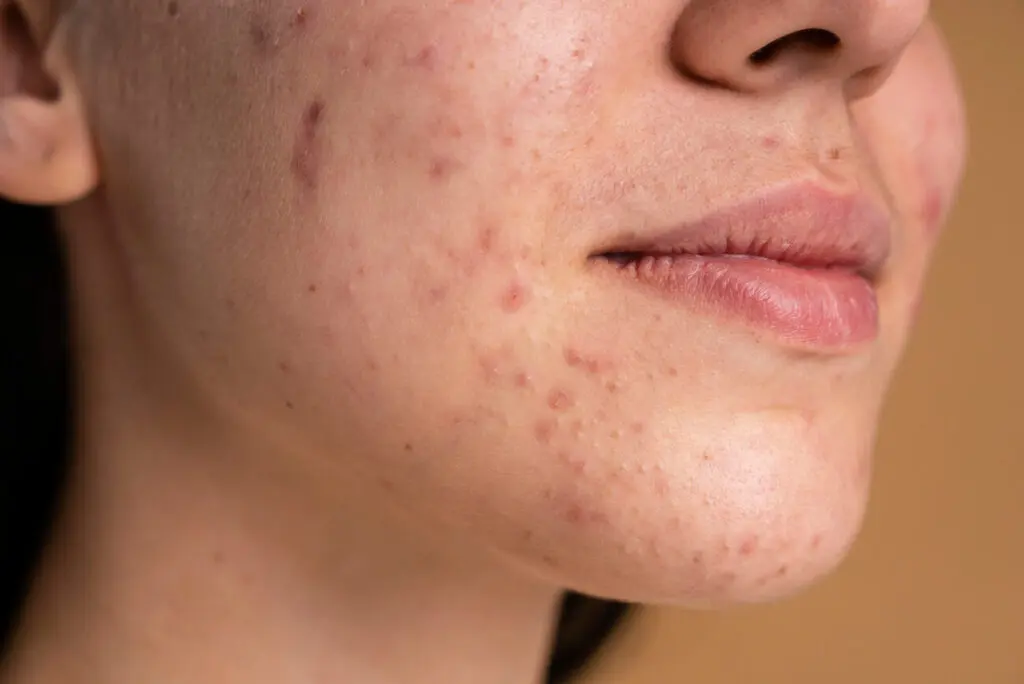
Adult acne can present in several forms, depending on its severity and underlying causes.
The most common lesions include blackheads and whiteheads, which are non-inflammatory, as well as papules and pustules, which are inflamed and may feel tender to the touch. In more severe cases, deeper nodules and cysts can develop beneath the skin and are often painful.
Adult acne most often appears on the lower part of the face, particularly the jawline and chin, although it can also affect the cheeks, neck, chest, and back.
Alongside visible breakouts, patients may notice ongoing redness, skin sensitivity, and marks that remain after spots have healed. Post-inflammatory hyperpigmentation is particularly common and can persist long after the active acne has cleared.
If the condition is not managed appropriately, repeated inflammation may increase the risk of scarring, which can be more difficult to address than the acne itself.
What Causes Adult Acne?
Adult acne develops as a result of several biological processes that affect the skin’s oil production, cell turnover, and inflammatory response.
One of the key factors is increased sebum production. Sebum is a natural oil that helps protect the skin, but when it is produced in excess, it can contribute to blocked pores. At the same time, dead skin cells may accumulate and fail to shed properly, further clogging the hair follicles.
This creates an environment in which bacteria, particularly Cutibacterium acnes, can multiply. The immune system responds by triggering inflammation, which leads to the visible redness, swelling, and discomfort commonly associated with acne.
Hormonal activity plays a significant role in adult acne. Androgens, a group of hormones present in both men and women, can stimulate the oil glands and increase sebum production. Even subtle hormonal changes can have a noticeable effect on the skin.
Genetic predisposition may also contribute, meaning some individuals are naturally more prone to developing acne under certain conditions.
In most cases, these factors do not act in isolation. Adult acne is usually the result of several overlapping influences, rather than a single identifiable cause.
6 Key Triggers That Can Worsen Adult Acne

While the underlying causes of adult acne are biological, certain triggers can make the condition more noticeable or persistent. Identifying these factors is often an important step in managing breakouts more effectively.
The most common triggers include:
1. Family History
Genetic factors can influence how the skin produces oil and responds to inflammation. Individuals with a family history of acne may be more prone to developing adult acne or experiencing more persistent symptoms.
2. Hormonal Fluctuations
Hormonal changes remain one of the most significant triggers. Many patients notice flare-ups linked to their menstrual cycle, pregnancy, or perimenopause. These shifts can increase oil production and affect how the skin behaves over relatively short periods.
3. Stress and Cortisol Levels
Stress does not directly cause acne, but it can make existing symptoms worse. Higher cortisol levels may increase oil production and contribute to inflammation. In addition, stress can influence sleep and daily habits, which can indirectly impact skin health.
4. Skincare and Cosmetic Products
Some skincare and cosmetic products can clog pores or irritate the skin, particularly if they are not labelled as non-comedogenic. Using too many active ingredients, such as exfoliating acids, may also disrupt the skin barrier and lead to increased sensitivity and breakouts.
5. Diet and Lifestyle Factors
There is growing evidence that diet may play a role in acne for some individuals. High glycaemic foods, such as refined carbohydrates, may contribute to breakouts. Some people also notice a link between dairy products and acne. These triggers vary from person to person, so patterns are best assessed individually.
6. Medications and Underlying Conditions
Certain medications, including corticosteroids and lithium, are known to trigger acne-like symptoms. Hormonal conditions such as polycystic ovary syndrome (PCOS) may also contribute to persistent adult acne and may require further medical evaluation
How Adult Acne Is Diagnosed
Adult acne is usually diagnosed through a clinical assessment carried out by a dermatologist. This involves a close examination of the skin to understand the type of lesions present, their severity, and how they are distributed across the face or body.
Alongside the physical examination, a detailed medical history is often discussed.
In some cases, further evaluation may be recommended. This is more likely if the acne is persistent, severe, or associated with other symptoms that suggest an underlying hormonal or medical factor. For example, hormonal imbalances may be considered if acne is accompanied by irregular cycles or other related changes.
It is also important to distinguish adult acne from other skin conditions that can appear similar, such as rosacea or folliculitis, as these require different approaches to treatment.
From a clinical perspective, adult acne is managed within dermatology, alongside a range of common skin conditions. A thorough assessment allows treatment to be tailored to the individual and their specific skin needs.
Treatment Options for Adult Acne

Effective treatment for adult acne depends on several factors, including its severity, underlying causes, and individual skin characteristics. For this reason, a tailored approach is usually required rather than a single standard solution.
Topical Treatments
Topical therapies are often the first step in managing adult acne, particularly in mild to moderate cases. Retinoids are commonly used as they help normalise cell turnover, reducing the likelihood of blocked pores over time. Benzoyl peroxide works by reducing acne-causing bacteria and inflammation.
Other options include topical antibiotics, which are typically used for inflammatory acne, and azelaic acid, which can help both with breakouts and post-inflammatory pigmentation. These treatments are often combined to improve overall effectiveness while minimising irritation.
Oral Medications
For more persistent or moderate to severe acne, oral treatments may be recommended. Antibiotics can help reduce inflammation and bacterial activity, although they are usually prescribed for limited periods.
Hormonal therapies may be appropriate in cases where acne is linked to androgen activity, particularly in women. In more severe or treatment-resistant cases, isotretinoin may be considered under specialist supervision.
Professional Dermatology Treatments
In a clinical setting, additional treatments may be used to support medical therapy. These can include chemical peels, which help improve skin texture and unclog pores, as well as laser or light-based therapies that target inflammation and bacteria.
Such treatments are usually part of a broader management plan rather than standalone solutions, and are selected based on individual skin needs and treatment goals.
Skincare and Daily Management
Alongside medical treatments, a consistent and balanced skincare routine plays an important role. This typically includes gentle cleansing, appropriate moisturisation, and the use of non-comedogenic products designed for acne-prone skin.
Overly harsh or complex routines can disrupt the skin barrier and may worsen irritation, so a simple and consistent approach is often more effective. Sun protection is also important, particularly when using active treatments that can increase skin sensitivity.
The key point is that there is no single treatment that works for everyone. Looking at acne within the context of overall skin health allows for a more comprehensive and effective approach. It also helps ensure that related concerns, such as pigmentation or scarring, are addressed in a timely and appropriate way.
In practice, managing adult acne often involves a combination of treatments, carefully tailored to the individual’s skin, lifestyle, and underlying causes. Also, it is important to note that most treatments require several weeks to show visible improvement, and consistency plays a key role in achieving long-term results.
When to Seek Professional Help
Professional advice should be considered when adult acne persists despite over-the-counter treatments, becomes painful, or leads to scarring. These signs can indicate that the condition would benefit from a more targeted, medical approach.
Early assessment is often helpful, as it can prevent the acne from progressing and reduce the risk of long-term skin changes, including scarring and pigmentation.
Support may also be beneficial if acne is affecting confidence or overall quality of life. Dermatological care is not limited to severe cases and can be valuable at any stage, particularly when breakouts are recurrent or difficult to manage independently.
For those experiencing persistent or recurrent adult acne, a consultation at London Lauriston Clinic can provide a clearer diagnosis and a structured, personalised treatment plan. Each treatment plan is developed following a detailed assessment, focusing on underlying causes, managing active breakouts, and supporting long-term skin health.
Frequently Asked Questions About Adult Acne
Can adult acne go away on its own?
Mild cases may improve without treatment, but persistent adult acne often requires targeted care to prevent worsening or scarring.
Why does adult acne appear around the jawline and chin?
This area is more sensitive to hormonal changes, which can increase oil production and lead to breakouts.
Can stress cause adult acne?
Stress does not directly cause acne, but it can worsen it by increasing oil production and inflammation.
Is adult acne linked to diet?
Some evidence suggests high glycaemic foods and dairy may trigger acne in certain patients, though this varies.
What is the most effective treatment for adult acne?
Treatment depends on the cause and severity. Options include topical treatments, oral medication, and clinical procedures.
When should adult acne be assessed by a specialist?
If acne is persistent, painful, or not improving with basic treatments, a specialist assessment is recommended.
Can adult acne cause scarring?
Yes, particularly if it is severe or untreated. Early treatment helps reduce this risk.
Is adult acne linked to other skin conditions?
It can occur alongside other skin conditions, which is why a full dermatological assessment is often useful.
What is the difference between adult acne and rosacea?
Adult acne typically involves blackheads, whiteheads, and inflamed spots caused by clogged pores and excess oil. Rosacea, on the other hand, is a chronic condition characterised by persistent redness, visible blood vessels, and sometimes small bumps, without blackheads.
Conclusion
Adult acne is a common condition, but one that benefits from a clear and considered approach. Its causes are often multifactorial, triggers can differ from person to person, and effective treatment depends on understanding these individual factors rather than relying on general advice.
While many cases can be managed with appropriate skincare and targeted medical treatment, persistent, recurrent, or more severe acne is best assessed by a specialist. Early, tailored intervention can help improve outcomes and reduce the risk of longer-term skin concerns.